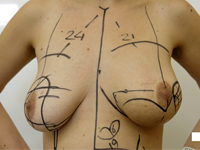
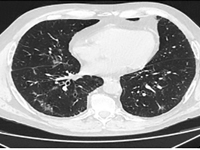
SARS-CoV-2 infection in a patient with adenocarcinoma with a mutation in the EGFR gene treated with erlotinib - a case report
Lung cancer accounts for the largest number of cancer deaths worldwide [1]. Despite advances in treatment, incidence and mortality rates continue to rise. A 2018 GLOBOCAN analysis reported 2.09 million new cases of lung cancer and 1.76 million deaths from lung cancer worldwide [2]. There are two main histological types: small cell lung cancer (DRP) and non-small cell lung cancer (NDRP). NDRP accounts for about 85% of all lung cancer cases. It includes various subtypes such as adenocarcinoma, squamous cell carcinoma and large cell carcinoma. The most common subtype is adenocarcinoma accounting for 45% of NDRP cases. The most important risk factor for developing lung cancer is smoking, especially among the male population. The use of filtered cigarettes, which reduce the amount of tar entering the lungs, correlates with an increase in the incidence of lung adenocarcinoma, which is associated with stronger inhalation of carcinogens into the fine airways. Other compounds that may have an effect on cancer development are asbestos, radon, nickel, cadmium, chromium, silica and arsenic. The development of molecular studies at the beginning of the 20th century made it possible to identify the genetic basis of the disease by demonstrating the presence of mutations or rearrangements of TP53, MYC, BCL2 genes in small cell carcinoma and EGFR, KRAS, MET, BRAF, NTRK, ROS1, ALK, RET, PIK3CA genes in non-small cell carcinoma [3]. The percentage of non-squamous NDRP patients with mutations in the gene for the epidermal growth factor receptor (EGFR) is 10-15 (in Caucasian patients) to more than 40% (in Asian patients) [4]. A deletion in exon 19 and a substitution at codon 858 (L858R) in exon 21 account for 80-90% of mutations within the tyrosine kinase coding domain of the EGFR gene [4]. Lung cancer manifests as cough, hemoptysis, chest pain, shortness of breath and/or hoarseness. In the case of adenocarcinoma, brain metastases manifesting as headache, vomiting, visual field disturbances, seizures or neurological deficits are common. After appropriate laboratory and imaging tests and histopathological evaluation, it is possible to assess the histological type and stage of the cancer. Depending on the patient's general condition, tumor stage and concomitant diseases, different treatment methods are used. For low-grade cancer (stages I, II and IIIA), surgery is used, often in combination with chemotherapy and radiation therapy. For stage IIIB patients, the therapy of choice is chemoradiotherapy, and if chemoradiotherapy is not available, the treatment is the same as for patients with generalized NDRP. Therapy for patients with distant metastases (stage IV) is aimed at reducing the discomfort and symptoms of progressive disease and prolonging life. For this purpose, chemotherapy, immunotherapy or molecularly targeted therapy are used [5]. Molecularly targeted therapy for lung cancer with EGFR gene mutations is made possible by the use of tyrosine kinase inhibitors (IKTs). IKTs inhibit intracellular phosphorylation of EGFR which leads to the arrest of cell differentiation, proliferation and angiogenesis. EGFR IKTs are divided into three generations. Erlotinib and gefitinib are the first-generation reversible IKTs. They are effective in the presence of the most common mutations in exon 19 and 21. Second-generation irreversible IKTs, which include afatinib and dacomitinib, show a broader spectrum of action. They block the transmission of signals formed by ErbB1 (EGFR), ErbB2 (HER2), ErbB3 and ErbB4 receptors, and can be effective in the presence of rare mutations in exons 18, 19, 20 and 21. It is possible to acquire resistance to first- and second-generation IKTs. Ozymertinib, an irreversible third-generation IKT, by acting on cells with the T790M mutation in exon 20 of the EGFR gene, overcomes resistance to treatment with older-generation EGFR IKTs, but can also be used in 1st-line treatment in NDRP patients regardless of the type of mutation in exons 18-21 of the EGFR gene [6]. The global COVID-19 pandemic poses a therapeutic challenge to healthcare, especially among oncology patients. A retrospective analysis from Wuhan showed that the risk of COVID-19 infection was 2.31 times higher among cancer patients than in healthy individuals. Smoking, age, male gender, cancer status, poor performance status (≥2 on the ECOG scale) and treatment with hydroxychloroquine with azithromycin were risk factors for increased 30-day mortality among COVID-19 patients [7]. Hospital visits during the pandemic and the use of immunosuppressive medications are major contributors to COVID-19 infection in lung cancer patients [8]. A study conducted in China, showed that NDRP patients over 60 years of age are particularly vulnerable to COVID-19 infection and a more severe course of the disease. Many respiratory symptoms in COVID-19 i.e. shortness of breath, cough, fever overlap with those of lung cancer. This creates a difficulty in differential diagnosis between the two disease entities. The diagnosis of COVID-19 is usually made on the basis of clinical history and PCR test and/or antigen test in a sample from nasopharyngeal secretions. Recognition of typical lesions seen on chest CT scan is also helpful. Multifocal opacities of the frosted-glass type with predilection for the lower lobes are present in 75% of patients [9]. A study conducted in New York among lung cancer patients with concurrent SARS-CoV2 infection showed the need for hospitalization in 62% of patients, 21% of whom required ICU hospitalization. Of the 102 patients participating in the study, 25% died. Survival was more dependent on the comorbidity of COPD (chronic obstructive pulmonary disease) and smoking than on tumor histology or PD-L1 (programmed death ligand 1) expression on tumor cells [10].
Received 05 May 2021→Accepted 07 Dec 2021→Published 08 Dec 2021