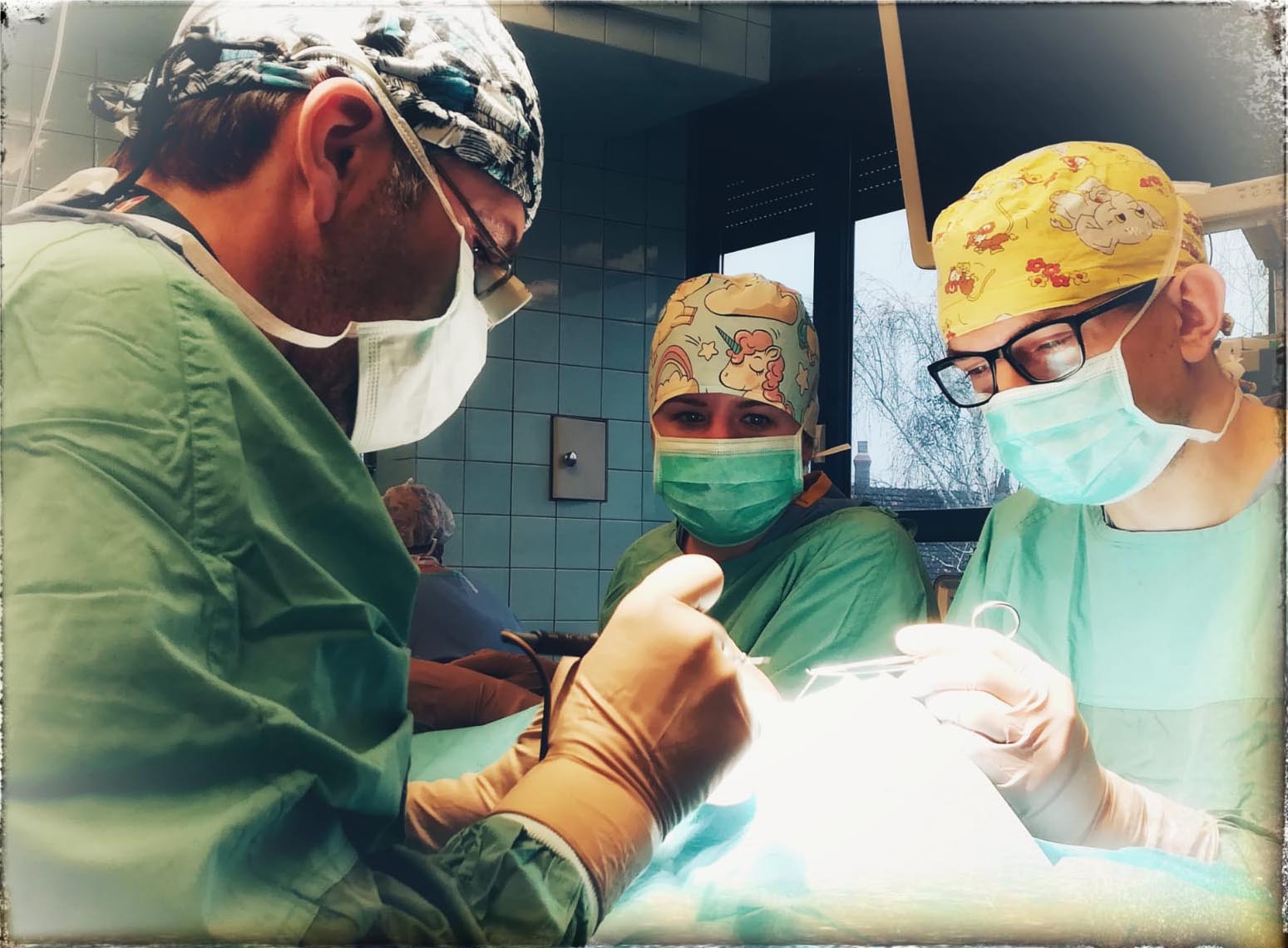
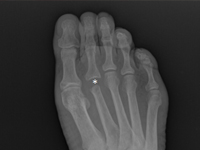
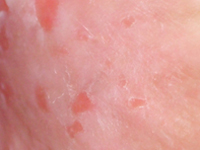
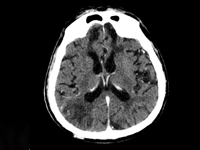
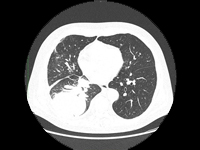
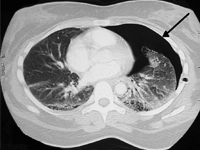
Example of management of metatarsal bone II tumor originally suspected of having metastatic thyroid follicular cancer 40 and 20 years after total thyroidectomy
Known There are many causes causing discomfort and nodular lesions in the metatarsal area and forefoot. They include These include traumatic soft tissue injuries i bones (e.g., sole plate tears, toe arthritis, arthritis, fractures fatigue, Freiberg fracture), tendon diseases (e.g. tendinosis, tendon sheath inflammation, tendon rupture), non-cancerous soft tissue lesions (e.g., ganglion, bursitis bursitis, granuloma, Morton's neuroma), and, less commonly, tumors and their metastases to soft tissues and bone [1]. Focal bone lesions are often an incidental result of imaging. Alternatively, they may be the cause of pain, a palpable mass or a fracture pathological [2].Most often patients associate these symptoms with trauma. In fact, trauma only draws attention to the the affected area, but does not cause the formation of a tumor. [5] In all these cases, especially in the early stages, accurate diagnosis is crucial, to establish further differential diagnosis and treatment strategy, so when confronted with a focal bone lesion, it is necessary to follow a logical management algorithm. First, it should provide description of the lesion in correlation with the patient's age, location, type of bone, cortical involvement, periosteal reactions, the condition of the adjacent soft tissue. W this for this purpose, it is necessary to x-ray of the involved area in two projections with adjacent joints. A deeper diagnosis is achieved by CT examination, assessing the advancement of the bone lesions and MRI, infiltrating adjacent soft tissues . If imaging studies show more advanced disease, an important diagnostic element is to obtain material for pathomorphology, taken during open biopsy or oligobiopsy, and establish the histological diagnosis [11]. W case of confirmation of a neoplastic process, it is always necessary to perform a examination X-RAY/CT chest, ultrasound/ CT of the abdomen, or even PET to exclude metastases [5]. The second step of the implemented algorithm dictates that treatment should be planned based on the answers to the following questions: - Is the lesion likely to be a normal variant, That is, "leave me alone, don't touch me," a lesion of a benign type, requiring no further imaging or supplies, but only observation? [3] - Does the lesion have features suggestive of an aggressive nature, and then whether further imaging is necessary, which technique best to use, whether a biopsy of the lesion is required and advanced treatment? [4]. Heterogeneity clinical picture of unidentified focal nodular lesions w metatarsal and forefoot, the variety of available methods of diagnosis do not make the task any easier, both at the stage of making the initial diagnosis, as well as during communication between members of the interdisciplinary team, which many times should deal with address treatment. The purpose of of this article is to present a similar situation using the case of a tumor of the distal epiphysis of the second metatarsal bone as an example, suspected of late, distant metastasis of thyroid cancer, never not confirmed in further studies, and suggestions for management diagnostic and therapeutic management. Cancer Follicular The thyroid gland (FTC - Follicular Thyroid Carcinoma) accounts for 10-20% of of all cancers of the thyroid gland. It is the second most common encountered thyroid cancer [6], and metastasis to the metatarsal bones and fingers are extremely rare.