Publications
Peer-reviewed clinical case reports
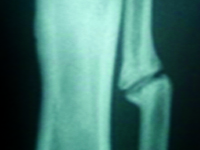
Staw rzekomy w wyniku złamania trzonów kości podudzia u dziecka – opis przypadku
Pseudoarthrosis after tibia and fibula shaft fracture in a child – case report
GynecologyJest to rzadki przypadek, w którym pierwotnie zdiagnozowane przerzuty FTC do kości śródstopia nie zostały potwierdzone w dalszej diagnostyce. W związku z tym wykonano jedynie resekcję guza. Diagnostyka pooperacyjna opierała się na wielokrotnych, dokładnych badaniach histopatologicznych wycinków pobranych w trakcie operacji, co wykluczyło niekorzystne rozpoznanie. Dzięki temu uniknięto amputacji stopy.
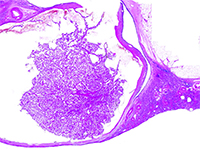
Rak nerki związany z nabytą torbielowatością nerek - nowa jednostka w klasyfikacji WHO 2016. Opis dwóch przypadków wykrytych na wczesnym etapie rozwoju.
Acquired cystic disease associated renal cell carcinoma - new entity in classification WHO 2016. Report of two cases detected at an early stage of development.
SurgeryW 2012 roku The International Society of Urological Pathology (ISUP) zaproponowało wdrożenie do klasyfikacji 5 nowych podtypów raka nerki, w tym raka nerki związanego z nabytą torbielowatością nerek (ang. acquired cystic disease - associated renal cell carcinoma - ACD-RCC). W 2016 roku ACD-RCC został uznany za niezależną jednostkę w Klasyfikacji Nowotworów Układu Moczowego WHO 2016. [1]. Poniższa praca prezentuje typowe cechy ACD-RCC w oparciu o dwa przypadki.
Problemy diagnostyczne oraz postępowanie terapeutyczne w przypadku neurokiły
Diagnostic problems and therapeutic procedures in the case of neurosyphilis
Internal MedicineCurrently, syphilis is a growing epidemiological problem, as evidenced by the growing number of new infections, also in Poland [1]. A negative phenomenon is the increasing incidence of late-stage Treponema pallidum infections, including syphilis of the central nervous system (CNS) [2]. In advanced stages of syphilis, and especially in neurosyphilis, the risk of permanent complications increases, including tenesmus dorsi, progressive paralysis, stroke, and others [3]. CNS syphilis poses a significant diagnostic challenge because the symptoms of infection can mimic other primary CNS diseases or systemic diseases with secondary CNS involvement. Therefore, it is often called "the great imitator" [4, 5, 6, 7].
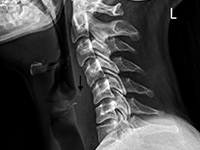
Ciało obce tkanek miękkich szyi - opis przypadku
Foreign body of the neck - case report
OtherForeign body ingestion is more common in children than in adults, but serious complications are less common in pediatric patients [1, 2]. Among adults, elderly individuals, those with masticatory disorders, esophageal strictures, prisoners, and patients with mental disorders predominate [2-4]. 80-90% of swallowed foreign bodies pass through the upper gastrointestinal tract spontaneously, but 10-20% require endoscopic removal, and 1% cause complications [3,5]. Possible locations of foreign bodies in the midpharynx include the epiglottis, the base of the tongue, the palatine tonsils, and in the hypopharynx, the piriform recesses, the retrocricoid region, and the posterior pharyngeal wall [6, 7]. In the esophagus, foreign bodies are located in the cervical part in over 80% of cases [1, 2, 8]. It is rare for a swallowed foreign body to penetrate the gastrointestinal tract and migrate deep into the soft tissues. This may be facilitated by the foreign body's structure, e.g., sharp-edged pieces of bone or glass. This poses a risk of serious and potentially fatal complications, such as retropharyngeal abscess, mediastinitis, or damage to the large vessels of the neck [7]. In such cases, prompt intervention and removal of the foreign body are essential. We present the case of a patient with a foreign body that migrated from the hypopharynx into the soft tissues of the neck, directly adjacent to the common carotid artery.
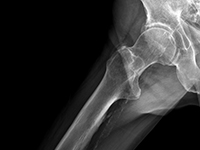
Nawrót pierwotnie niezdiagnozowanej polimialgii reumatycznej (PMR) po 6 latach od wystąpienia pierwszych objawów
The recurrence of an originally undiagnosed polymyalgia rheumatica (PMR) 6 years after its first symptoms occurrence
SurgeryPolymyalgia rheumatica (PMR) is one of the most common rheumatic diseases diagnosed in people over 50 years of age. Its incidence increases with age, reaching a peak at 72-73 years of age (PMR is rarely diagnosed in the 50-year-old population) [1]. Statistically, it affects women twice as often. A greater predisposition is also observed in the white race [2]. In Europe, the incidence is on average 1 in 133 people over 50 years of age [3]. There is also a clear geographical variation – the vast majority of diagnoses occur in Northern European countries, particularly Sweden, while in Southern Europe, for example, in Italy, it is much less frequently diagnosed. The etiology of the disease has not been fully elucidated. It is assumed that autoimmune processes underlie it. The role of solar radiation and viral infections has also been suggested [2]. Typical symptoms of polymyalgia include pain and stiffness in the neck, shoulder girdle, and hip muscles [1,2]. PMR belongs to a group of inflammatory diseases with an immune basis. Its etiology also includes a genetic predisposition, including the involvement of antigens: HLA-DR4, HLADRB1*04, and proinflammatory cytokines: TNFα and IL6. Some studies have also demonstrated reduced secretion of adrenal cortex hormones (cortisol, dehydroepiandrosterone) in individuals affected by this condition [4]. The variety of factors postulated to play a significant role in the development of PMR indicates the need for further research into the etiology of this disease.

Abstrakty - 7 Kongres Europejskiego Stowarzyszenia Dziecięcych Chirurgów Endoskopowych
Abstracts - ESPES (European Society of Paediatric Endoscopic Surgeons) 7th Annual Congress
OtherIt is my great pleasure to present a special edition of our Journal, printed for the occasion of the 7th Annual Congress of the European Society of Paediatric Endoscopic Surgeons (ESPES)! In this issue you can find regular case reports submitted to the Journal and all abstracts of ESPES 2017 Congress (September 27th — 29th Wroclaw, Poland). Professor Dariusz Patkowski, a member of our Scientific Council, is the Congress Chairman. All abstracts will be also available after Congress on the journal’s website — www.MDcase.net.

Wewnątrzmaciczne zahamowanie wzrastania płodu w przebiegu Zespołu Silver-Russella - opis przypadku
Intrauterine growth restriction in the course of Silver-Russell syndrome - a case report
Internal Medicine<p>Intrauterine fetal growth restriction (IUGR) is one of the most serious complications of pregnancy. It affects an average of 8% of live-born newborns in developed countries, and up to 15-20% in developing countries[1, 2, 3].</p><p>It is associated with an increased rate of intrauterine deaths and pregnancy complications, including preterm deliveries and perinatal deaths. In children, abnormalities in psychophysical development and a higher incidence, including in adulthood, of conditions such as obesity, diabetes, and metabolic syndrome are observed[1, 2, 7, 8 , 9]. IUGR refers to the inability of the fetus to reach its full growth potential during intrauterine life [4, 5, 6]. Many times the term hypotrophy is used interchangeably. According to most authors, IUGR is diagnosed when two ultrasound measurements of the fetus show excessively slow growth rates and/or when birth weight/length is less than 2 SD ( standard deviations), or 10th percentile relative to gestational age. In severe forms, birth weight or AC ( abdominal circumference) correspond to values below the 3rd Centile. [6, 8]. The etiology of intrauterine growth retardation is multifactorial, and despite advances in medicine, it is often, even in 40%, impossible to identify . We distinguish maternal causes ( among others.: hypertension, kidney disease, cardiovascular disease, diabetes mellitus, thrombophilias, antiphospholipid syndrome, genetic factors, drugs), fetal(mainly genetic abnormalities, congenital malformations, intrauterine infections, metabolic blocks), placental (abnormalities in placental structure and capacity, pre-eclampsia), environmental (low socioeconomic status of the mother, stimulants, nutritional deficiencies) [1, 9, 10, 11, 12].</p><p>The management of suspected IUGR should include a thorough general medical and obstetric history, assessment of risk factors to identify pregnant women requiring enhanced surveillance, and detailed imaging and laboratory tests. Ultrasonography of the fetus (evaluation of anatomy, size , proportion, growth dynamics) is the primary diagnostic test. It is also necessary to monitor fetal well-being with cardiotocography (ktg), assessment of blood flow in selected vessels ( usg doppler), amniotic fluid volume and biophysical profile. Appropriate laboratory tests are performed to confirm or exclude maternal chronic diseases, intrauterine infections, pre-eclampsia, HELLP syndrome and other pregnancy pathologies that may affect growth disorders [12,13]. In the absence of a clear cause leading to IUGR, genetic testing is important. Maternal genes are believed to have a major impact on the baby's birth weight. However, also many chromosomal aberrations in the fetus are associated with intrauterine growth retardation [6, 12]. An example is Silver- Russell syndrome (SRS), which varies widely in the type of genetic alterations present and how they are inherited. Mutations affect chromosome 11, 7, among others, and are associated with characteristic phenotypic features, which include primarily bone lesions in the form of : scoliosis, limb length disproportion, toe fusion, elbow joint lesions. According to the literature, between 1:50,000 and 1:100,000 children are born with this syndrome [14, 15, 16].</p><p>The main goal of maternal and child care in pregnancy complicated by intrauterine fetal growth retardation is to ensure and strictly assess fetal well-being and to choose the optimal delivery date [6, 12].</p>.

Przypadkowo wykryty rak języka u pacjenta z niedokrwistością i bólami stawów.
Tongue cancer diagnosed incidentally in a patient with anaemia and joint pain.
SurgeryTongue cancer is the most common oral cancer [1]. Most patients report exposure to known risk factors for cancer development, such as frequent alcohol consumption, smoking, and poor oral hygiene [1, 2]. Unfortunately, due to the tumor's location and patients' failure to appreciate early symptoms, most diagnoses are made in very advanced stages of the disease [2]. We present a case report of a patient with incidentally diagnosed tongue cancer.
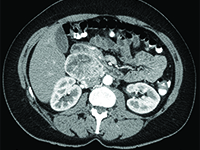
Przyzwojak u 41-letniej kobiety - rzadki nowotwór przestrzeni zaotrzewnowej
Paraganglioma in a 41-years old woman: a rare neoplasm of the retroperitoneal space
Gynecology<p>Paraganglioma(Latin: paraganglioma) is a rare, mostly benign neuroendocrine tumor originating from the paraventricular bodies of the parasympathetic and sympathetic nervous systems. The 2013 National Cancer Registry did not find any data on the incidence of this tumor in Poland [1]. The histopathological structure and symptoms of the tumor often resemble pheochromocytoma. It can be said that pheochromocytoma is a special type of chaperone tumor. Chaperones originating from the parathyroid bodies of the parasympathetic nervous system are usually located near the large vessels of the head and neck (bifurcation of the common carotid artery-the most common location) [2], while chaperones from the sympathetic nervous system chaperones occur along the sympathetic trunk located adjacent to the vertebral column, abdominal aorta and inferior vena cava [even aortic glomerulus (Zuckerkandel's organ) lying on either side of the aorta, just above its bifurcation-the most common location].</p><p>Parenomas are neoplasms of old age, with peak incidence in the 5th and 6th decades of life. In about 10% of cases, they occur familially, being part of such genetically determined syndromes as [3]:</p><p>- von Hippel-Lindau syndrome</p><p>- multiple endocrine adenocarcinoma syndrome types 2A and 2B</p><p>- Carney syndrome</p><p>Diagnosis of chaperones is not straightforward, as these tumors are rare. In cases where the tumor is hormonally active, there are symptoms associated with high levels of catecholamines in the blood (accelerated heart rate, increased blood pressure, hot flashes, headaches). When a hormonally active tumor is absent, symptoms may result from tumor growth in a specific location (dull pain in the lumbar region). Most often, however, chaperones are diagnosed incidentally in a neck or abdominal and pelvic ultrasound performed for other reasons or as an annual prophylaxis (the tumor diagnosis is then confirmed on CT).</p><p>Tumor fine-needle biopsy is unlikely to be performed due to the rich vascularization of the tumor and the associated risk of bleeding.</p><p>Because of the rarity of chaperones, there are no established diagnostic and therapeutic algorithms.</p><p>Treatment consists of surgical removal of the tumor. In cases where the location of the tumor does not allow surgical removal, radiation therapy is applicable.</p><p></p><p>Rocalization is generally very good. If the tumor is completely removed, the cure is complete.</p>
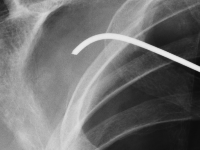
Ciało obce w klatce piersiowej
A foreign body in the chest
GynecologyPatients with pneumothorax constitute a significant percentage of all hospitalizations in general surgery departments. Pneumothorax can be spontaneous, most often caused by pulmonary emphysema, or post-traumatic, primarily resulting from chest wall contusion. A specific type of pneumothorax is the iatrogenic variety, which can generally be classified as post-traumatic.
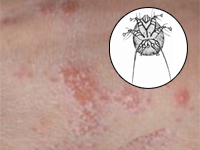
Ciężki przypadek świerzbu u biorcy przeszczepu nerki mylnie interpretowany jako skórne zmiany alergiczne.
Severe scabies misdiagnosed as allergic reaction after kidney transplantation.
SurgeryDue to immunosuppressive therapy, paƟents who underwent organ allotransplantaƟon are more likely to present an unusual clinical manifestaƟon of frequent everyday diseases. We present an uncommon case of Scabies in the renal transplanted recipient.
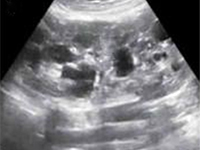
Zespół móżdżkowo-pozapiramidowy jako nietypowa manifestacja zespołu Gitelmana u rodzeństwa
Cerebellar-extrapyramidal syndrome as unusual manifestation of Gitelman syndrome in siblings
OtherIt’s a case presentaƟon of two siblings: a 17-year-old girl and her 15-year-old brother who both developed speech and swallowing difficulƟes, shaking hands and decreased muscle tone at the age of 4. Results of laboratory tests only indicated a tendency to low potassium and magnesium serum concentraƟons. The siblings were diagnosed for cerebellar-extrapyramidal syndrome. AŌer several years of follow-up the paƟent were referred to the Pediatric Nephrology Hospital because of hyperechogenic reflecƟons from renal parenchyma in abdominal ultrasound. Finally, tubulopathy was diagnosed. Diet supplements was included as a result of a persistent electrolyte imbalance, with a posiƟve therapeuƟc effect.