Publications
Peer-reviewed clinical case reports
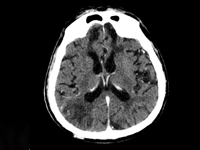
Gdy Twój pacjent śpi za dużo, czyli zaburzenia świadomości u pacjenta geriatrycznego – opis przypadku
When your patient sleeps too much, disturbance of consciousness in the case of a geriatric patient – case report
Internal MedicineIn The world, including Poland, has seen a systematic increase in the share of the general population of elderly people. The aging of the population and the associated increase in the number of geriatric patients now represents another of the challenges to be met by 21st century medicine. Patient A geriatric patient, as defined by the WHO (World Health Organization Organization), is a patient who has reached at least 60 years of age. The person under study is usually accompanied by a significant amount of illness, which is typical of old age and coexists with the risk of sudden deterioration of health or death [1]. In line with the need, a number of solutions are being implemented around the world, leading to the to improve the branch of medicine that is geriatrics. Comprehensive assessment geriatric assessment (Comprehensive geriatrc assessment, CGA) is a tool that consists of a set of scales and tests that allow a holistic assessment of patients facilitating the detection of the cause of deterioration and the selection of optimal therapy. A complete patient assessment, depending on the patient's clinical condition, takes between 30 to 60 minutes [2]. Comorbidities and medications taken by geriatric patients geriatric patients often require significant modification of generally accepted standards of treatment. A large number of emergencies in elderly patients proceed with disturbances of consciousness. Difficulties in correctly perceiving the of the surrounding world that patients encounter greatly complicate the the ability to accurately take a medical history, as well as conduct a physical examination and implement appropriate diagnostic and therapeutic measures.
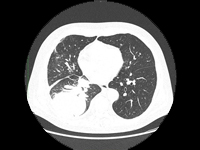
Możliwości leczenia systemowego u chorych na NDRP po przeszczepie narządów - opis przypadku i przegląd literatury
Possibilities of systemic treatment in patients with NSCLC after organ transplantation - case report and literature review
SurgeryThe introduction of antibiotics, mass vaccinations to prevent infectious diseases and organ transplants can be considered the greatest achievements of 20th century medicine. Solid organ transplants save the lives of patients suffering from organ failure and improve their quality of life. The life expectancy of transplant patients has improved significantly over the past two decades. Successful transplantation improves survival in patients on chronic dialysis and in patients with irreversible liver, heart and lung disease and end-stage failure of these organs. The percentage of transplants performed is steadily increasing, but is still insufficient [1]. According to data reported to the Global Observatory on Donation and Transplantation (GODT), 106,879 organ transplants were performed in 95 countries worldwide in 2010, including:73,179 kidney transplants (46% from living donors), 21,602 liver transplants (15% from living donors), 5582 heart transplants, 3927 lung transplants, 2362 pancreas transplants and 227 small bowel transplants. This activity increased by 2.12% compared to 2009 [2].Unfortunately, it is estimated that the number of transplants performed is insufficient. At the same time, there are huge geographic differences in the number of transplants per million population: from 70 per million population in developed countries to 0-2.4 in developing countries [3]. As transplantation prolongs patients' lives, cancers are becoming an increasing threat to long-term survival, especially in patients who have undergone liver transplantation for hepatocellular carcinoma (HCC)[4].The risk of cancer in transplant patients is higher than in the general population. This is due to three reasons. Immunosuppressive treatment accompanying organ transplantation causes a decline in immunity, which can promote infection with oncogenic viruses such as humanpapillomavirus (HPV) or humanherpesvirustype 8 (HHV-8), and can allow emerging cancer cells to escape from weakened immune surveillance. In addition, immunosuppressive drugs have a cytotoxic effect, which can induce the formation of mutations and the transformation of normal cells into cancer cells. Therefore, patients undergoing organ transplantation most often develop hemato-oncologic malignancies, cancers associated with infection with potentially oncogenic viruses: Kaposi's sarcoma (infection with human herpes viruses), cervical cancer and squamous cell carcinomas of the head and neck region (infection with human papillomavirus), liver cancer (infection with hepatitis B and C viruses) and skin cancers. Lung cancer, cancers of the gastrointestinal tract or urinary tract occur in no more than 1% of transplant recipients. The feasibility of using systemic cancer treatment in organ transplant patients has yet to be explored. The most controversial is the use of immunotherapy in cancer patients previously undergoing organ transplantation and immunosuppressive treatment. Modern cancer immunotherapies targeting immune checkpoints are designed to enhance the immune response, and thus may increase the risk of transplant rejection. Lung cancer is one of the leading causes of death from malignant tumors worldwide. There are two main types of lung cancer: non-small cell lung cancer (NDRP) and small cell lung cancer (DRP). NDRP is much more common, accounting for 80-85% of lung cancer cases. Thoracic surgery, chemotherapy and radiation therapy have been used to treat lung cancer [5]. Due to unsatisfactory treatment results, the search for new therapies began. The use of immunotherapy and molecularly targeted therapies proved to be a breakthrough. These therapies have been successfully used in selected patients with locally advanced and metastatic NDRP. These therapies have led to an increase in disease progression-free time and overall survival of patients, allowing lung cancer to be classified as a chronic disease [6].
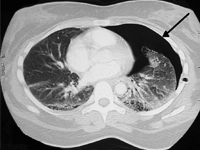
Nawracająca odma opłucnowa w przebiegu mukowiscydozy – trudności terapeutyczne. Opis przypadku.
Recurrent pneumothorax in course of cystic fibrosis – treatment challanges. Case report.
GynecologyCystic fibrosis (cystic fibrosis) is the most common genetic disease with autosomal recessive inheritance among the Caucasian population. The incidence varies from country to country. In Poland, it is about 1/2300 of live births. In its course, as a result of mutations on both copies of the CFTR (cystic fibrosis transmembrane conductance regulator) gene, which encodes a chloride channel, ion transport in all exocrine glands is disrupted, leading to dysfunction of key organs for survival, such as the pancreas, liver, lungs and intestines [1].Respiratory complications are the first cause of premature death in CF patients. Pulmonary manifestations of CF include hemoptysis, pneumothorax, chronic sinusitis and airway inflammation, bronchial dilatation, and respiratory failure, among others. Pneumothorax is the presence of air in the pleural cavity. Risk factors are associated with chronic infection with Burkholderia cepacia and Pseudomonas aeruginosa and the coexistence of other complications such as hemoptysis and pancreatic insufficiency [4]. Significant disease progression (FEV1 30%) [2] also favors the occurrence of this complication. Taking into account the criterion of time, we can distinguish the first case of emphysema, or recurrent emphysema, when the air leak reappears within 7 or more days after the previous episode. If the air leak persists for 5 or more days, we can recognize persistent emphysema (Shidlow 1993). Therapy can be divided into medical (oxygen therapy and observation) or surgical interventions. The latter group, which includes drainage, pleurodesis and pleurectomy depending on the course of treatment, is considered a more effective therapeutic option for patients with emphysema without significant concomitant lung disease. However, in CF-affected patients, it may complicate the lung transplant procedure in the future. There are no clinical trials available that reliably compare the efficacy and risk of complications of both types of interventions in CF patients [3-4]. An additional complication is that emphysema recurs in 50-90% of these patients, and in almost half of them it also occurs on the opposite side of the chest. Emphysema significantly worsens lung function, and the patient experiences shortness of breath and significant pain. If refractory to treatment, it is an independent indication for lung transplantation.[5]Here we present the case of a 16-year-old female patient with recurrent unilateral pneumothorax, in which, due to the severity of the disease, the diagnosis and therapeutic measures taken were fraught with numerous problems.
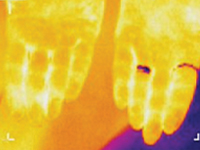
Termosemiotyka przewlekłego zapalenia migdałków
Thermosemiotics of chronic tonsillitis
Internal MedicineResearch Objective – to develop thermosemiotics of chronic tonsillitis by determining specifics of infrared waves in the submandibular region and on the palms, knees and in the center of foot vault in healthy people and comparison of the obtained results with the corresponding indices of patients with chronic tonsillitis. Most common pathogens in infectious tonsillitis are Streptococcus spp. Tonsillitis infrequently develops on the background of acute respiratory disease, but usually manifests itself as a separate disease. Suppression of local immune response on cold exposure, malnutrition, physical exhaustion, blockage of nasal pathways by adenoid tissue, chronic sinusitis, deviation of the nasal septum, chronic rhinitis are favorable set ssup for tonsillitis formation [1-3]. In clinical practice, it is often necessary to distinguish acute tonsillitis from chronic, because they are fundamentally different diseases. Recurrent acute tonsillitis that is frequently undertreated is commonly seen as preceding factor in development of chronic tonsillitis. Follicular form of tonsillitis is considered most unfavorable as it leads to scar formation in lymphoid tissue therefore diminishing its protective properties. Tonsillolith are formed consisting of desquamated epithelium, microbes, inflammatory exudate. They are difficult to evacuate and causing lacunar expansion, formation of retention cysts [4, 5]. Tonsilitis is notorious for its complications, such as myocarditis, rheumatic diseases, nephritis. Exacerbation may occur on the background of chronic inflammatory process. Therefore, special attention needs to be directed to patient reported history, particularly frequency and duration of exacerbations. Exacerbation of chronic tonsillitis is accompanied by symptoms of general intoxication – subfebrile temperature, pain in joints, decreased tolerance to physical exertion, fatigue. The tonsils, as a rule, are enlarged, have submucosal purulent follicles (however, in the absence of signs of acute tonsillitis, hyperemia and inflammatory infiltration may be present), caseosus-purulent masses in cicatricial lacunae. Regional lymph nodes are enlarged, dense, sometimes painful. Tonsil-cardial syndrome is often observed with subjective sensations of pain in the region of the heart, heart intermission, palpitation. There may be vasomotor symptoms – pallor or hyperemia of the skin, xerodermia or increase perspiration functional heart murmurs, myocarditis [4].Research Objective – to develop thermosemiotics of chronic tonsillitis by determining specifics of infrared waves in the submandibular region, on the palms, in the projection of kneecaps, and in the center of foot vault both in patients with chronic tonsillitis and healthy persons.
Czy zawsze udaje się ustalić etiologię ostrego zapalenia trzustki? Rzadki przypadek kliniczny OZT u chorej z erytromelalgią pierwotną
Can the etiology of acute pancreatitis always be identified? A rare case of acute pancreatitis in a patient with primary erythromelalgia
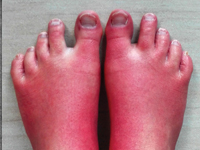
SurgeryAPD is the most common pancreatic disease and also a quite frequent cause of hospitalization of patients presenting to the hospital for due to abdominal pain. There has been an increasing incidence in recent years in developed countries and mortality in this disease reaching 5%. [1, 2]. Accurate diagnostics should make it possible to determine the etiology of UTI in more than 96% of cases [3] this, however, is still not achieved in many patients this is not achieved. Thus, relapse may occur with reoccurrence of a previously unrecognized etiologic factor. Many authors raise the role of drugs as a potential causative factor of ICS of unclear etiology[4]. There is no strictly defined regimen for effective yet safe treatment of pain in ICS. To date, it has not been established to what extent the drugs used for pain relief in this disease may simultaneously be a causative factor in pancreatitis[5, 6]. Primary erythromelalgia (EM), is a rare, genetically determined disease manifested by pain in the extremities, their increased heat and redness [7] [Image 1 - Painful erythema of the extremities lower extremities is the most common symptom in patients with Primary Erythromelalgia]. Treatment pharmacological treatment of this disease is not always effective. Various physical and invasive methods, including neurolysis of the lumbar segment of the sympathetic trunk sympathetic trunk [8]. This causes patients with EM often overuse pain medications, some of which are also used in the symptomatic treatment of pain in EM. We present the case of a 25- year-old EM patient who developed symptoms of ICS 10 days after unsuccessful pharmacological neurolysis of the lumbar sympathetic trunk and was preceded by the use of several analgesics, later also used in the treatment of during treatment of pancreatitis. Despite thorough diagnostics, it was not possible to determine the cause of the OST
Pacjent z wielonaczyniową chorobą wieńcową i schyłkową niewydolnością nerek leczony wielokrotnymi przezskórnymi interwencjami wieńcowymi.
Patient with multivessel coronary artery disease and end-stage renal disease treated with multiple percutaneous coronary interventions.
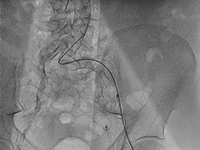
SurgeryEnd-stage renal failure (SNN) is a growing problem in developed countries [1]. Although diabetes remains the most common cause of dysfunction of these organs [2], chronic nephropathy can also be caused by autoimmune diseases, particularly from the vasculitis group. In the United States, the number of patients with SNN requiring dialysis therapy already reaches nearly 500,000, and more than 200,000 are living with an active kidney transplant [3]. Chronic kidney disease (CHD) is a significant cardiovascular problem, contributing to the rapid development of coronary artery disease coronary artery disease, especially the multivessel form. The more severe course of coronary artery disease coronary artery disease in patients with PChN is influenced by impaired calcium metabolism and a tendency to diffuse arterial calcification [4]. Patients with PChN and high CRP levels are at particularly high risk of cardiovascular incidents [5,6]. Currently, there are no guidelines for the surgical treatment of coronary artery disease in patients with PChN. However, they have a higher risk of death after revascularization than in the population without PChN [7]. Opinions on the effectiveness of of using percutaneous coronary intervention (PCI) and coronary artery bypass grafting (CABG) are divided, and there are no conclusive data in this regard. There are also no recommendations suggesting the development of a long-term strategy for treating coronary artery disease in patients with SNN, although it has been it has been described that they require multiple repeat PCI (if this method is chosen method) [8].
Skręt esicy u nastoletniego pacjenta
Sigmoid volvulus in an adolescent male patient
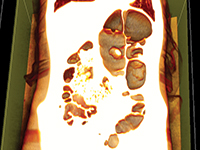
GynecologySigmoid volvulus (SV) is a condition where sigmoid colon twists or torsions about its mesentery. This disorder is rare in infants and children[1]. It usually occurs in adults, after the age of 40, more commonly in males[2]. SV leads to intestinal obstruction, which is often acute in children, whereas in adults it may be subacute or progressive. As a result of intestinal obstruction, the most common symptoms include abdominal pain, distention, vomiting and, in chronic cases, constipation. In Europe, Australia and the United States, the incidence of SV is very low. Nevertheless, SV remains the leading cause of acute colon obstruction in developing countries[3]. The diagnosis is based on clinical and radiological findings and is more difficult to establish in children compared to adults[4], and a correct diagnosis can be easily missed or delayed[4]. We present a case report with exceptional quality CT images and 3D reconstructions.
Migracja złamanego drutu Kirchnera po zespoleniu zwichniętego stawu barkowo-obojczykowego – opis przypadku.
Migration of a Kirschner wire used in fixation of acromioclavicular joint dislocation – case report.
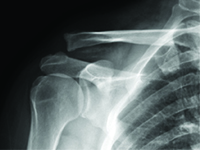
GynecologyDislocation of the acromioclavicular joint refers to complete or partial misalignment of the articular surfaces of the neighbouring scapula and clavicle [1]. It is an injury which often occurs in contact sports, such as football, judo, rugby and many more. It is also a relatively common injury in daily activities, as a result of falling during a walk or falling off a chair with impact on the shoulder girdle [2], [3].<br />Depending on the grade of the injury, recommended approaches vary from conservative treatment (grade I and II) to surgical treatment (above grade III).<br />Conservative treatment recommendations are: cooling, painkillers and limb elevation. Surgical treatment consists of surgical stabilisation of the dislocation. There are many techniques and methods to fixate the injury, including: Kirschner wires, using TightRope, double Endobutton, MINAR, Copeland and Kessel, Waver and Dunn or dedicated plates [3], [4].<br />
Nawrót przepukliny przeponowej u 21 letniego mężczyzny – opis przypadku.
Recurrence of diaphragmatic hernia in a 21-year-old man - case report.
SurgeryCongenital diaphragmaƟc hernia (CDH) is a developmental defect consisƟng in the dislocaƟon of abdominal organs into the chest. The displacement occurs through a hole in the diaphragm formed during the fetal period. The recurrence of diaphragmaƟc hernia is rare and appeared most oŌen aŌer a few weeks aŌer surgery.

Wpływ diety wegetariańskiej na INR u pacjentki leczonej antykoagulantami
Effect of vegetarian diet on INR in patient treated with anticoagulants
Internal Medicine<p>Warfarin sodium (Latin: Warfarinum natricum), found under the trade name Warfin, is an effective anticoagulant used in the prevention and treatment of thrombosis. It is widely used after cardiac surgery, especially after implantation of an artificial heart valve prosthesis. Warfin's role is to prevent blood from clotting in the prosthesis and valve components and to help dissolve any clots that form.</p><p>Patients must continue anticoagulant treatment for the rest of their lives. They also remain under the constant medical care of the cardiology clinic. In general, they should monitor the prothrombin time (PT), or the time of blood clot formation, every 4-6 weeks to see how the clotting factors that go into the so-called prothrombin syndrome are working. The result is presented under the name International Normalized Ratio (INR) (<i>Enternational</i><i>Normalized Ratio)</i> [1]. In order to maintain stable blood density values, patients should adhere to a well-balanced diet, thus ensuring that the body receives the recommended daily dose of vitamin K contained in foods. Too high a dose of vitamin K in relation to the body's needs can significantly affect the INR value in the blood tested and create difficulties in selecting the antivitamin K dose [2].</p><p></p><p>There are three classified forms of vitamin K: K1 and K2 - derived from a natural source, and K3 which is a synthetic chemical compound. Vitamin K1 (phylloquinone) is synthesized exclusively in plants and taken with food, while K2 is a group of compounds known as menaquinones (MK-n) [3]. These compounds are synthesized by intestinal bacteria. They are mainly found in animal products, including those that are fermentable (Table 1).</p><p>Table 1.</p><p>Recommendations from the FAO (<i>Food and Agriculture Organization of the United Nations</i>) and WHO (<i>World Health Organization</i>). <i>World Health Organization), </i>for sufficient intake of AI (<i>Adequate</i><i>Intake</i>), expressed in μg of phylloquinone/os/d since 2008, have not changed and are 65 μg of phylloquinone/os/d for women ≥ 19 years of age while 55 μg of phylloquinone/os/d for men ≥ 19 years of age [5]. It is now accepted that the therapeutic INR for anticoagulant treatment in patients after artificial valve surgery should be in the range of 2.5 - 3.5 regardless of gender [6, 7]. The clinical efficacy of Warfin depends on the plasma vitamin K concentration, which is influenced by the amount of vitamin K ingested through food and from supplementation. The U.S. government agency FDA (<i>English </i><i>Food and Drug</i><i>Administration)</i> reports that a daily vitamin K intake of 400 μg or more can completely nullify the anticoagulant effects of Warfin taken by the patient [8, 9].</p><p>Selecting the right vitamin K-containing foods and distributing them in meals is a major challenge for the dietitian. Taking into account the patient's general condition and his or her age, gender, weight, comorbidities, other medications and supplements he or she is taking, as well as specific behavioral behaviors (diet, exercise), the dietitian can properly tailor an individual nutrition plan for a specific patient. The more information the nutritionist receives, the more accurate the result of his work will be. Green parts of vegetables and fruits are characterized by a high content of vitamin K1 (phylloquinone), so when establishing a diet plan for a patient, this factor should be taken into account first and foremost.</p><p></p><p>Vitamin K is also involved in bone metabolism. Long-term use of Warfin may disrupt the homeostasis of calcium metabolism in the patient's body, resulting in osteopenia and, consequently, osteoporosis. However, these are remote consequences. Additional factors such as age, gender, physical activity, genetic conditions may contribute to their occurrence [10].</p><p>An important element is the absorption of vitamin K in the body. The absorption of phylloquinone requires the cooperation of bile and pancreatic juice. It is a fat-soluble vitamin, so adding it to a meal results in higher absorption. Vitamin K is absorbed in the small intestine and is stored in the liver. There are differences between the absorption of vitamin K1 and K2. The former is absorbed only 10-15% of the total amount of this vitamin taken in with food, while K2 is absorbed almost completely and has a long biological half-life [10]. In the overall picture, vitamin K modifies coagulation stability, but it should not be excluded from the patient's diet because it is essential for the normal functioning of the human body. In addition to its involvement in the process of blood coagulation, it is involved in the maintenance of proper bone tissue homeostasis and in the proper functioning of the nervous system and brain function.</p><p></p><p>It can be assumed that a properly balanced dietary plan will contribute to the maintenance of normal concentrations of coagulation factors when confronted with anticoagulants and minimize fluctuations in the blood coagulation index.</p>
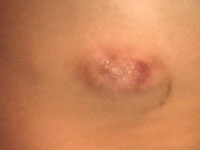
Maska skórna anaplastycznego chłoniaka wielkokomórkowego
Anaplastic large cell lymphoma hidden by skin lesion
OtherNon-Hodgkin's lymphomas are a group of diseases caused by neoplastic transformation of lymphoid cells. Anaplastic large cell lymphoma (<i>Anaplastic large cell lymphoma; </i><i>ALCL)</i>ALK+ (<i>anaplastic lymphoma kinase (ALK)-positive ALK+)</i>. is a neoplasm that originates from T lymphocytes. ALK is a tyrosine kinase receptor with an as yet undiscovered ligand so-called "orphan" (<i>orphan receptor</i>). Activation of of abnormal transmission is caused by a translocation involving the 2p23 region. ALK activation is thought to activates the STAT3, AKT/PI3K, RAS/ERK pathways responsible for cell proliferation and the cell cycle. The occurrence of ALCL ALK+ is relatively rare. It occurs in 3% of adult non-Hodgkin's lymphoma patients and in 10-15% of pediatric lymphoma patients. ALCL ALK+ is an aggressive lymphoma. It is mostly found in younger people (median age 34 years). It is more common in men than in women. The disease mainly occupies lymph nodes, but 60% of patients also have extranodal manifestations. The ALCL ALK+ staging classification uses the Ann Arbor classifications are used. Within 5 years of treatment, 60% of patients remain free of disease recurrence. [1]
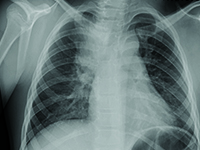
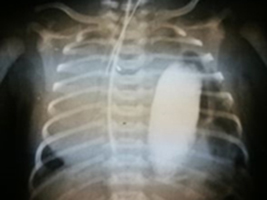
Wrodzona wada układu oddechowego wykryta u 9-letniej dziewczynki z zapaleniem płuc
9 years old girl with pneumonia and congenital defect of pulmonary truct
OtherDefects Congenital defects are abnormalities of the structure of organs created before birth, which lead to dysfunction of these organs. It is estimated that the formation of birth defects birth defects are influenced by: toxic-environmental factors (in 5-10%) and genetic factors (in 20-25%), but in 70-80% no cause can be determined. The incidence of all congenital malformations of congenital malformations in newborns and infants is about 4%, less than 4% of them (about 3.9%) involve the respiratory system. Nearly half of children with congenital defects of the respiratory system die before the age of five. Symptoms of defects in the respiratory system of the respiratory system include chronic or recurrent respiratory infections, symptoms of respiratory failure, coughing, and hemoptysis. Sometimes a defect in the respiratory system of the respiratory system is asymptomatic and detected accidentally.